NeroVet AI dentistry uses machine learning to analyze dental X-rays and flag conditions like cavities, bone loss, and gum disease before they become severe. The technology works alongside dentists, not instead of them, giving clinics a faster second opinion and patients a more thorough, proactive approach to oral health.
Your dentist can only look at so many X-rays in a day before attention wavers. AI does not have that problem. In 2026, AI-assisted dental diagnostics has moved well past the pilot phase. Clinics in the U.S., UK, and across Europe are integrating these tools into daily workflows, and the evidence for early detection benefits is growing.
This article explains what NeroVet AI dentistry actually does, how the underlying technology works, what conditions it catches early, and what both patients and practice owners should expect from it.
What NeroVet AI Dentistry Actually Does
NeroVet AI dentistry is a category of software that applies trained machine learning models to dental image analysis and diagnostic support. The process is straightforward: a bitewing, periapical, or panoramic X-ray is fed into the system, and it returns a confidence-scored analysis with visual overlays highlighting suspected pathology.
The software does not replace the dentist. It works as a second reader, flagging areas of concern that the clinician then reviews, confirms, or dismisses. Think of it as a consistent, tireless assistant trained on hundreds of thousands of annotated radiographs.
In practice, this changes two things. Clinics process images faster and catch subtle findings earlier. Patients receive clearer explanations. Instead of describing an abstract shadow on a film, a dentist can show a color-coded overlay with annotations that point to a specific area of concern.
How AI Reads a Dental X-Ray
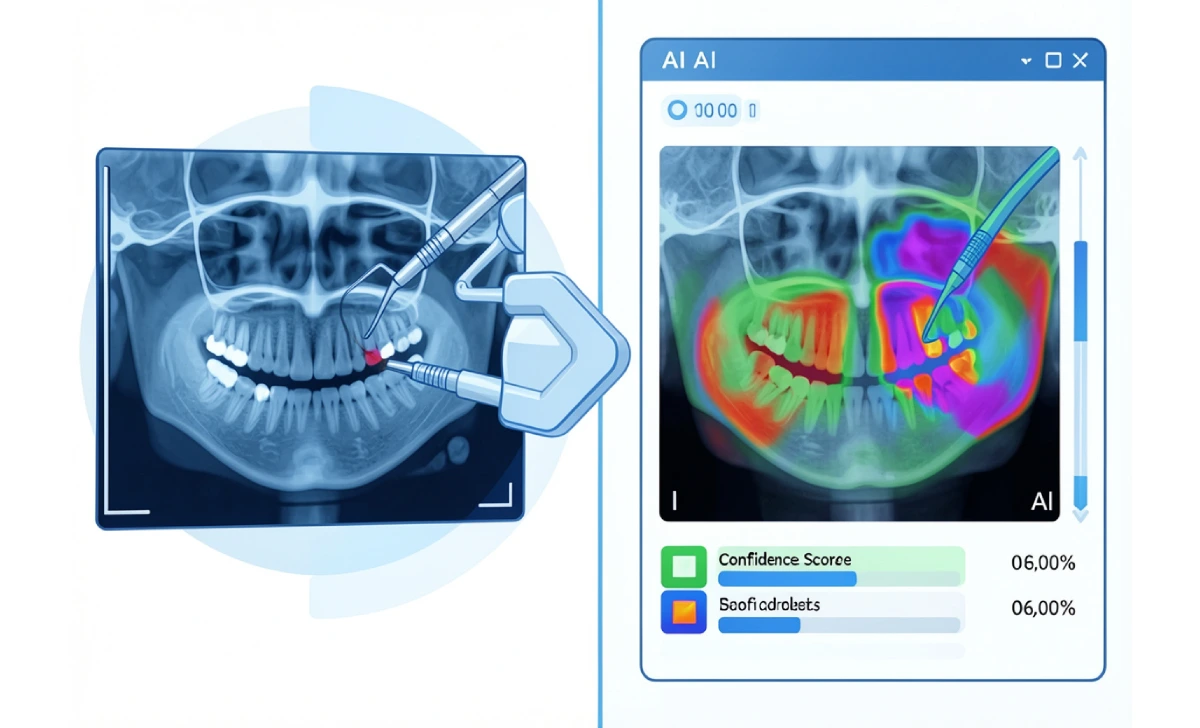
The core technology is a type of deep learning called a convolutional neural network (CNN). These models are trained on large datasets of dental radiographs where experienced clinicians have already labeled conditions: early caries, bone loss, root fractures, calculus, periapical lesions.
Once trained, the model learns which pixel patterns correspond to which conditions. When it receives a new X-ray, it compares what it sees against those learned patterns and outputs a probability score for each potential finding.
Speed is one of the most immediately visible advantages. Most AI dental tools return results in under five seconds. That is not marginally faster than manual review. It is a different order of magnitude, particularly when a dentist is working through a full-mouth series for multiple patients in a single session.
Early Detection: What NeroVet AI Dentistry Catches First
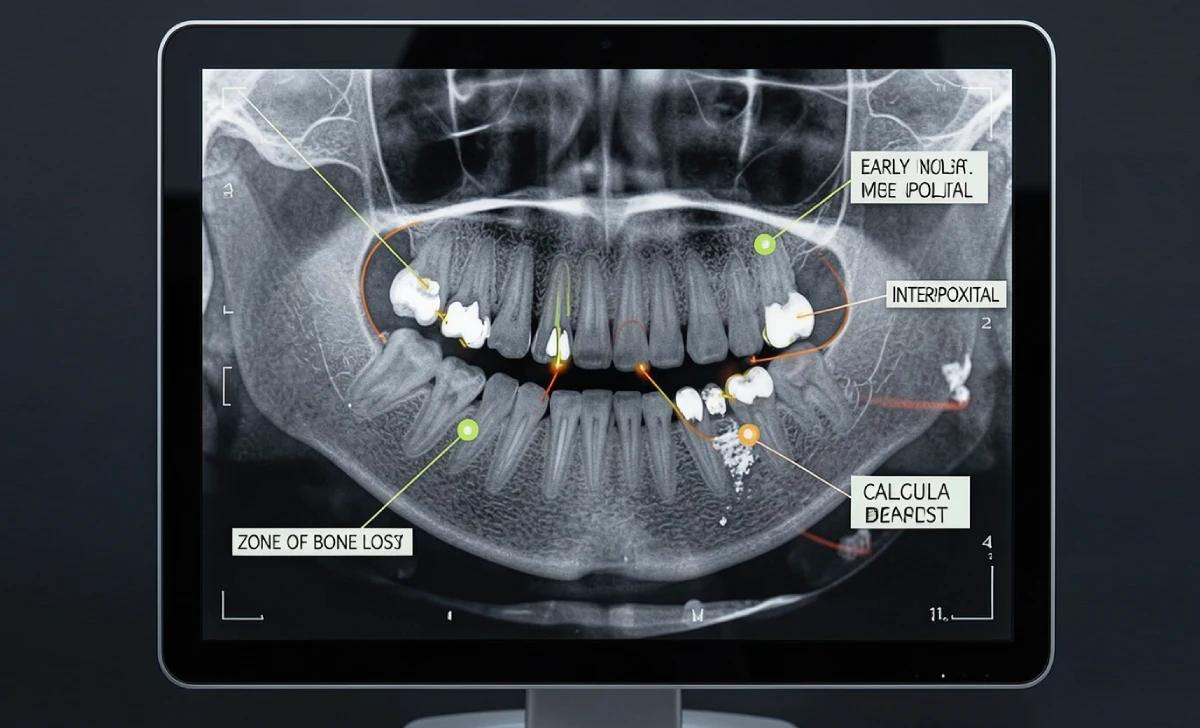
Cavities, Bone Loss, and Gum Disease
Early-stage cavities are easy to miss. Interproximal caries, which form between teeth, are particularly difficult to spot on a standard radiograph, especially when the lesion is still confined to the enamel. Research published in peer-reviewed dental journals has shown that AI systems trained for radiographic caries detection can match or exceed the performance of general practitioners for early interproximal lesions, the category where clinical misses are most common.
Bone loss associated with periodontal disease follows a similar pattern. AI tools measure bone levels consistently across a full-mouth series and flag progressive loss between visits. This removes subjectivity from a condition that is widely underdiagnosed in general practice.
Oral Cancer and Structural Abnormalities
Oral cancer screening has historically depended on visual and tactile examination. AI-assisted intraoral imaging adds pattern recognition that can flag suspicious tissue changes, abnormal densities, or lesions that warrant further investigation. Early detection of oral cancer has a direct impact on survival outcomes, which makes this one of the higher-stakes applications of the technology.
Beyond cancer, AI consistently picks up root fractures, periapical lesions, and calculus deposits that are easy to overlook in a busy clinical session. These findings rarely cause immediate symptoms but carry long-term consequences if left unaddressed.
AI’s Role in Treatment Planning
Detection is one part of what NeroVet AI dentistry contributes. The next part is what happens after a finding is confirmed.
AI platforms can simulate treatment outcomes based on existing diagnostic data. For implant placement, they overlay proposed positions onto a cone beam CT (CBCT) scan and check proximity to nerves, sinuses, and adjacent roots. For orthodontic cases, they model projected tooth movement and flag potential complications before treatment begins.
This has two practical effects. First, it reduces the margin for error in complex procedures by giving the clinician a data-backed reference point. Second, it gives patients a visual representation of what their treatment will involve and what the expected result looks like. Research consistently shows that patients who can see a treatment simulation are more likely to understand, accept, and follow through with complex care.
What Adoption Looks Like for Clinics
Bringing AI into a dental practice involves more than selecting software. Three real barriers apply to most clinics making this decision.
Cost and integration. AI dental tools typically charge per image or as a monthly subscription. Integration with existing practice management systems varies widely. Some platforms connect smoothly; others require manual upload workflows that add steps rather than remove them.
Staff training. Clinicians and dental teams need to understand what the AI is and is not telling them. A flagged finding is not a confirmed diagnosis. Practices need clear protocols for how AI output feeds into clinical decision-making and patient communication.
Data privacy and regulatory compliance. Patient radiographs are protected health information. Any platform handling this data must be HIPAA-compliant in the U.S. and GDPR-compliant in the EU. Clinics should verify compliance certification, data storage location, and breach notification protocols before committing to any tool.
Regulatory status is a separate consideration. In the U.S., dental AI tools used as diagnostic aids are subject to FDA oversight. Not all tools on the market have gone through that clearance process. Clinics evaluating platforms should confirm the regulatory status of the specific tool, not just the category of technology.
Accuracy, Limitations, and What AI Can’t Replace
Accuracy figures in vendor marketing typically range from 90% to 99%, depending on the study, the condition, and imaging quality. Independent research presents a more nuanced picture. Performance tends to be strongest for caries detection on bitewing X-rays and weaker for more complex findings like root fractures or early periapical lesions.
A few limitations apply consistently across AI dental tools:
- Output quality depends on image quality. A blurry or poorly positioned X-ray produces unreliable results regardless of the algorithm behind it.
- Training data shapes performance. A model trained on one population or imaging system may not generalize perfectly to different demographics or hardware configurations.
- AI cannot examine soft tissue directly, palpate lymph nodes, or take a patient history. The full clinical picture requires a human in the room.
What AI does consistently well is remove variability. A clinician seeing their 50th patient of the day may give that patient’s radiographs less careful attention than the first. The algorithm applies the same criteria to every image, every time.
Where Dental AI Is Heading
The current state of NeroVet AI dentistry is primarily retrospective: a patient comes in, an X-ray is taken, and AI reads it. The next phase involves continuous and proactive monitoring.
AI-enabled intraoral cameras, wearable oral sensors, and predictive models built on longitudinal patient data are in active development and early clinical deployment. The goal is to shift dental care from a problem-driven model toward continuous management, where changes in a patient’s oral health are tracked between visits and flagged before they require intervention.
For patients, this means fewer surprises at routine appointments. For clinicians, it means less time on routine screening and more time on complex diagnosis and care. For the technology to reach that potential, the volume of validated, independently verified training data needs to keep growing.
AI will not replace dentists. It will, however, continue to change what dentists spend their clinical time on. That shift is already underway.